Chronic Pelvic Pain
Chronic Pelvic Pain (CPP) is defined as persistent, noncyclic pain perceived to be in structures related to the pelvis, such as abdomen, pubic, perineum and rectal areas, that lasts more than six months. The pain can be severe enough to cause significant disability or require medical and/or surgical treatment that effects one’s quality of life.
The root cause of pain in CPP can be gynaecological, urological, gastrointestinal, musculoskeletal, psychoneurologic, or in most cases, a combination of those. There are many conditions that play a role in developing chronic pelvic pain but the 5 conditions that are most prevalent in CPP are Endometriosis, Interstitial Cystitis/Bladder Pain Syndrome, adhesions, Prostatitis and Irritable Bowel Syndrome.
When someone has lived with Chronic Pelvic Pain for many years, they may notice constant muscle tension and painful symptoms in other organs. CPP sufferers can feel lasting changes in their muscles that affect their bladder and their bowels.
Why do we feel pelvic pain?
The signals are sent down our spine to alert us to the dangers in our environment in order to protect ourselves. Once a person has long term (chronic) pain, the spinal cord “door” may be damaged. This may cause this “door” to stay open even after the diseased or injured tissue is healing. When this happens, the pain remains even though you treat the original cause. This is also known as Central Sensitization.
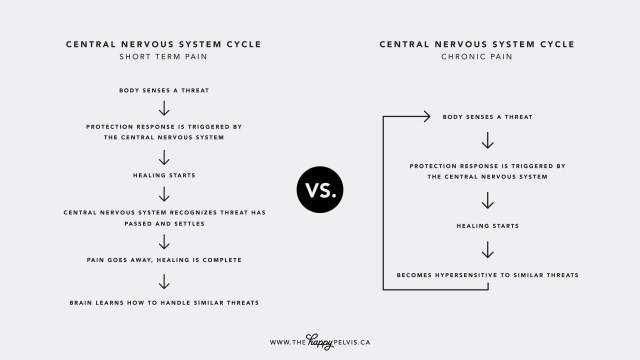
Short-term VS. Long-term Pain
When it comes to pain, there is short-term pain and chronic pain.
Short-term pain is the way our body tells us something is wrong and we should protect ourselves. An example of this is the pain you feel when touching a hot stove, or stubbing your toe, telling you to move away to protect yourself. Likewise, the pain you feel after an operation or injury tells you that you need to rest and allow your body to recover and heal. Short-term pain usually go away over time.
Chronic pain is when the pain doesn’t go away. The original cause of the pain may no longer be there. Infection or tissue damage can be nonexistent. There is nothing that needs medical attention immediately and you are in no danger. Tests may show no abnormalities. Yet, there is still pain. But why does this happen?
Central Sensitization in the Pelvis
It happens due to Central Sensitization, a term used for chronic pain. This means the nervous system goes through a wind-up process during painful episodes and gets regulated in a constant state of high reactivity. This process changes the way our bodies and brains perceive and react to pain triggers. The nerve endings can become so sensitive that they interpret any sensation, even pressure or inflammation, as pain.
As nerve pathways change and as they become more engrained in our brains and emotions, it’s much easier for our brains to perceive anything as a threat and continue to send pain signals, getting stuck in a vicious cycle.
Pain Management
In many cases, Chronic Pelvic Pain is not caused by one health problem but by a multitude of problems that are impacting each other. This means that many times there is not one single medication, treatment or therapy for CPP.
It is important to remember that some pelvic pain can never be completely cured and instead, you and your healthcare team’s goal should be to maximize quality of life.
You need to be realistic of your expectations and this may involve learning ways to build resilience and how to cope with pain flare-ups.
You are not alone. We’re in this together.
Ref.
Engeler DS, Baranowski AP, Dinis-Oliveira P, et al.; European Association of Urology. The 2013 EAU guidelines on chronic pelvic pain: is management of chronic pelvic pain a habit, a philosophy, or a science? 10 years of development. Eur Urol. 2013;64(3):431–439.
International Pelvic Pain Society. (2019, Aug 4). Basic Chronic Pelvic Pain. Retrieved from https://www.pelvicpain.org/IPPS/Patients/Patient_Handouts/IPPS/Content/Professional/Patient_Handouts.aspx?hkey=cffd598e-5453-4b3f-9170-457c59266b50. Accessed Mar 20, 2020.
LINDA M. SPEER, MD; SAUDIA MUSHKBAR, MD; and TARA ERBELE, MD, University of Toledo College of Medicine and Life Sciences, Toledo, Ohio Am Fam Physician. 2016 Mar 1;93(5):380-387.


















